World Diabetes Day India 2025: HbA1c, Prevalence & Future Outlook
India Faces a Growing Diabetes Crisis: A Call for Personalized Prevention
New Delhi – As World Diabetes Day is observed globally, India stands at a critical juncture in its battle against a rapidly escalating diabetes epidemic. What was once considered a disease of affluence is now impacting all socioeconomic strata, demanding a shift from reactive treatment to proactive, personalized prevention strategies.
The Scale of the Challenge
India’s diabetes prevalence has surged dramatically in recent decades. From approximately 32.7 million cases in 2000, the nation now grapples with nearly 89.8 million individuals living with the condition – an exponential increase fueled by lifestyle changes, urbanization, genetic predispositions, and evolving dietary habits. Alarmingly, the Centers for Disease Control and Prevention (CDC) estimates that 90-95% of cases are type 2 diabetes, largely preventable through lifestyle modifications.
However, the true extent of the problem may be even greater. Studies suggest that as many as 57 percent of adults with diabetes remain undiagnosed, highlighting a critical gap in early detection efforts. This delayed diagnosis often leads to complications, increasing the burden on individuals and the healthcare system.
A Nation of Contrasts: Regional Disparities
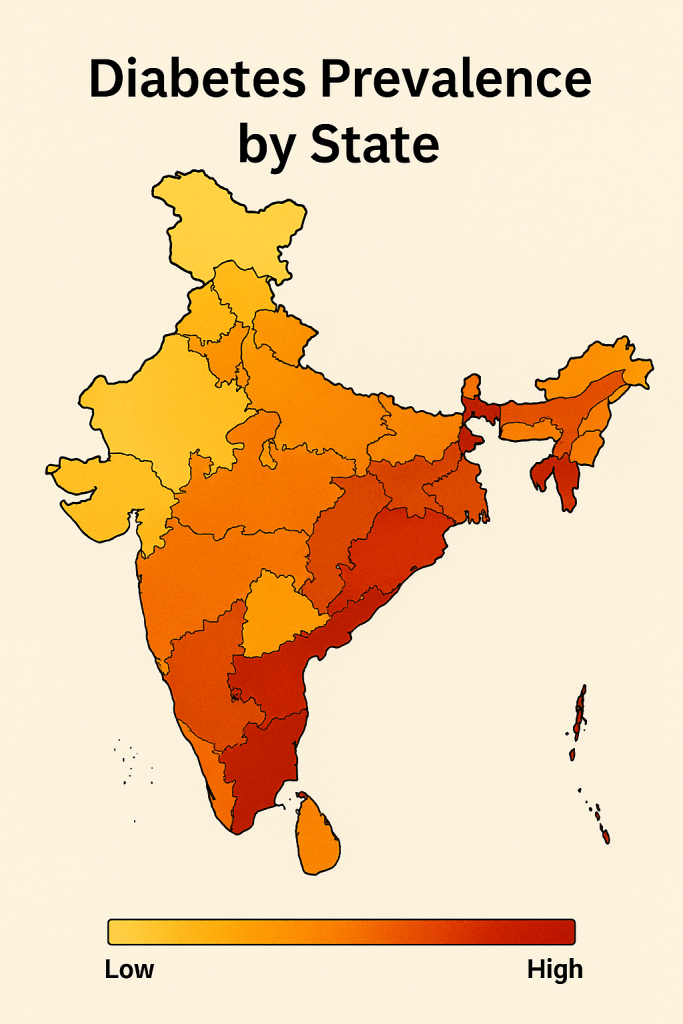
The diabetes landscape across India is far from uniform. States like Goa (26.4 percent prevalence), Puducherry (26.3 percent), and Kerala (25.5 percent) are experiencing particularly high rates, placing them among the most affected regions in the country. Conversely, states like Rajasthan (around 10 percent) and Bihar (as low as 4.3 percent in earlier surveys) exhibit lower prevalence, though this doesn’t necessarily indicate lower risk. Lower numbers can often reflect under-diagnosis, slower urbanization, and demographic differences.
Beyond prevalence, significant disparities exist in awareness and control. Meghalaya, for example, reports alarmingly low awareness levels of just 14 percent, while Telangana boasts rates exceeding 50 percent. This underscores the need for targeted public health campaigns and improved access to screening programs.
The ‘Thin-Fat’ Indian Phenotype and the Need for Precision Prevention
India faces a unique challenge with what experts call the “thin-fat” phenotype – individuals with normal body mass index (BMI) but high levels of visceral fat, increasing their risk of metabolic diseases like diabetes. This highlights the limitations of relying solely on BMI as a risk assessment tool. A one-size-fits-all approach to prevention is insufficient.
“We need to move towards precision prevention, built on Indian genetic and metabolic data, rather than simply importing Western models,” explains Dr. Anjali Sharma, a leading endocrinologist at All India Institute of Medical Sciences (AIIMS). “Our nutritional needs, exercise patterns, and risk factors are distinct, requiring tailored frameworks.” You can learn more about preventative health strategies on worldys.news.
Leveraging Technology and a Life-Course Approach
The future of diabetes management in India hinges on embracing technology and adopting a life-course approach. Remote monitoring, artificial intelligence (AI)-powered prediction models, wearable devices, and continuous glucose monitoring systems can facilitate continuous, personalized support, shifting the focus from episodic clinic visits to proactive health management.
Furthermore, addressing diabetes requires a holistic perspective that extends beyond middle age. Interventions must begin in childhood, encompassing school programs, corporate wellness initiatives, and policies that promote healthy food systems and urban design. Recognizing the strong link between diabetes and other chronic diseases – cardiovascular disease, kidney disease, and mental health – is also crucial.
Measurement, Accountability, and a Collective Responsibility
Effective diabetes control demands robust measurement and accountability. Simply tracking prevalence numbers is no longer sufficient. India must invest in metrics that capture time-in-range (the percentage of time blood glucose levels are within a target range), complication rates, workforce productivity, and quality-of-life indicators. High-burden states require advanced models focused on complication prevention, while lower-burden states present opportunities for early screening and lifestyle interventions.
Ultimately, tackling India’s diabetes crisis requires a collective effort – from individuals making informed lifestyle choices to policymakers implementing effective public health strategies. On this World Diabetes Day, the message is clear: prevention is not just a medical imperative, it’s a societal responsibility.