Rheumatoid Arthritis: Early Signs & Prevention of RA
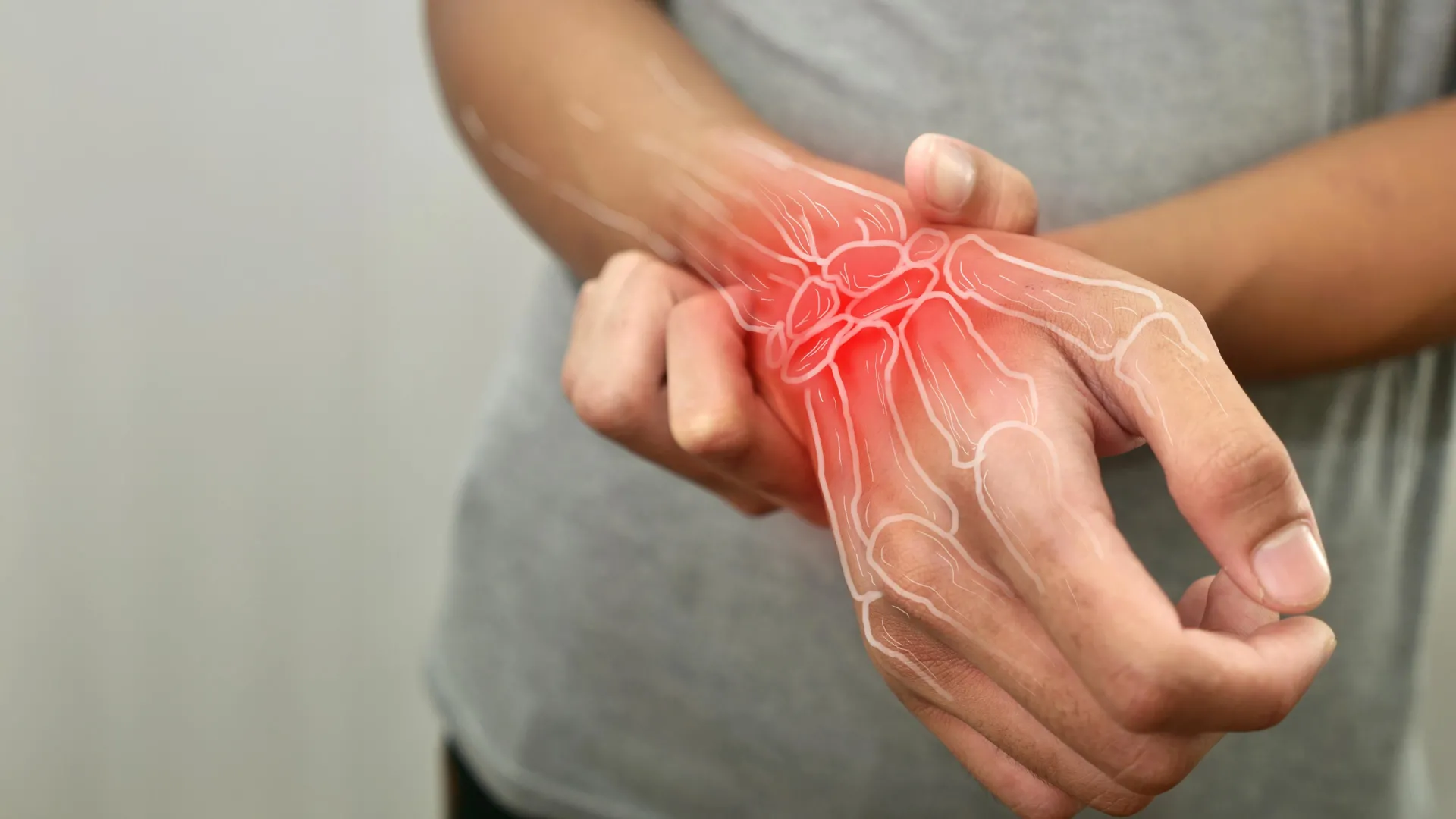
Rheumatoid Arthritis: Silent Years of Immune Activity Precede Joint Pain, Research Reveals
For years, doctors have focused on treating the visible symptoms of rheumatoid arthritis (RA) – the joint pain, swelling, and stiffness that can severely limit a person’s quality of life. But groundbreaking new research suggests the disease process begins much earlier, unfolding silently within the immune system long before a single ache appears. This discovery offers a potential paradigm shift in how we approach RA, moving from reactive treatment to proactive prevention.
Rheumatoid arthritis is a chronic autoimmune disorder affecting approximately 1.3 million adults in the United States, according to the Centers for Disease Control and Prevention. Globally, the prevalence is estimated at between 0.5% and 1% of the population. While the exact cause remains unknown, genetic predisposition and environmental factors are believed to play a role. The new findings, published in Science Translational Medicine, illuminate the complex immunological events that set the stage for the disease years in advance.
The Unseen Autoimmune Struggle
The multi-institutional study, a collaboration between the Allen Institute, CU Anschutz, University of California San Diego, and the Benaroya Research Institute, focused on individuals carrying ACPA (anti-citrullinated protein antibodies). These antibodies are a well-established biomarker, indicating an increased risk of developing RA. Researchers meticulously tracked these individuals over seven years, analyzing their immune activity to understand the earliest stages of disease development.
What they found was striking. Even in the absence of noticeable symptoms, these individuals exhibited widespread inflammation throughout their bodies – not just in the joints. This systemic inflammation mirrored the patterns seen in patients with active RA, suggesting the immune system was already engaged in a full-scale, albeit silent, autoimmune attack. “We’re seeing evidence that the body is already preparing for battle, even before the first sign of joint pain,” explains Dr. Kevin Deane, M.D./Ph.D. of CU Anschutz, a co-senior author of the study. “This opens up exciting possibilities for early intervention.”
Reprogramming the Immune System: A Cellular Level View
The research delved deep into the behavior of specific immune cells. B cells, responsible for producing antibodies, were found to be abnormally active, primed to launch an inflammatory response. T helper cells, crucial for coordinating immune responses, were also significantly expanded, particularly a subset called Tfh17 cells, known to contribute to autoantibody production. But perhaps the most surprising discovery was the observation of epigenetic changes in “naive” T cells – cells that hadn’t yet encountered any pathogens.
These epigenetic changes, alterations in gene regulation without changes to the underlying DNA sequence, suggested that these cells were being reprogrammed, essentially prepped for an autoimmune response. “It’s like the immune system is anticipating a threat and altering its defenses accordingly, even before a threat actually exists,” says Mark Gillespie, Ph.D., assistant investigator at the Allen Institute. Furthermore, monocytes, a type of white blood cell circulating in the bloodstream, were found to be producing inflammatory molecules, closely resembling the macrophages found in inflamed joints of RA patients. This indicates the immune system was already laying the groundwork for joint inflammation.
Implications for Early Detection and Prevention
The implications of this research are profound. Identifying these early immune signatures could allow doctors to pinpoint individuals at high risk of developing RA, even years before symptoms manifest. This would enable more frequent monitoring and, crucially, the potential to intervene with preventative therapies. Currently, treatment for RA focuses on managing symptoms and slowing disease progression. However, if the disease can be intercepted during this early, silent phase, it may be possible to prevent irreversible joint damage and significantly improve patient outcomes.
“The goal is to shift the paradigm from reacting to damage to preventing it altogether,” says Dr. Deane. “We need to identify potential biologic targets for preventing RA and develop strategies to improve treatments for those already diagnosed.” This research aligns with the broader global health focus on preventative medicine, championed by organizations like the World Health Organization, which emphasizes the importance of early detection and intervention to reduce the burden of chronic diseases. For patients, this offers a glimmer of hope – the possibility of a future where rheumatoid arthritis can be stopped in its tracks, before it has a chance to take hold.
For more information on autoimmune diseases and managing chronic conditions, explore resources available on worldys.news’ Health section.